Confusion Over Dry Eye Treatment
This variability in how we diagnosed a dry eye patient created confusion in knowing who really has dry eye symptoms from those who have true dry eye diagnosis. Why that’s important is because not all dry eye symptoms are genuinely from dry eye disease (this refers to co-conspirators that mimic dry eye disease). The flip side to that equation is that many patients could have dry eye disease manifestations without necessarily having true symptoms. With all this uncertainty, it was encouraging to see that the new Dry Eye Work Shop (DEWS II) from the Tear Film and Ocular Society was released with the focus on how to help clinicians better diagnose dry eye disease.

Now that we had a recommended approach to diagnosing dry eye disease with DEWSII, there remained several challenges that stood in the way of ensuring we achieve better success in dry eye diagnosis and management. In my opinion, the biggest challenge was not having a systematic and methodical way that is reproducible when we see a dry eye patient in the clinic. When you factor that we have to account for things like systemic medications a patient is on, weather, work environment, co-conspirators, as well as the ability to grade the variables we see on exam consistently, it becomes rather challenging to truly implement a practical approach in the clinic that allows a doctor to capture these variables consistently and assess them over time. This is especially important when we see that industry has been actively working on releasing many new therapeutic drugs and treatments for our dry eye patients to help address the rising prevalence of this disease. But without us being able to consistently capture all the various variables that can impact how someone really is doing with treatment, we as doctors and patients will find these new therapies potentially frustrating if we can’t measure their true effectiveness.
For all those reasons, there has never been a better time to ensure that we quantify dry eye disease in a consistent and practical way. Quantifying dry eye disease allows us to gather objective data that can guide our diagnostic and treatment pathways. This Data-Driven approach can be accomplished by using standardized questionnaires, point of care diagnostic tests, and using a more quantified method for how we traditionally document the severity of someone’s clinical findings. The results of these efforts will yield data that can help us stay objective in how we diagnose and manage dry eye diseases that are more in line with DEWSII recommendations. More importantly, by focusing on objective data gathering from our dry eye patients, we can better assess how a certain treatment is really working over time.

The Introduction of Dry Eye Technology
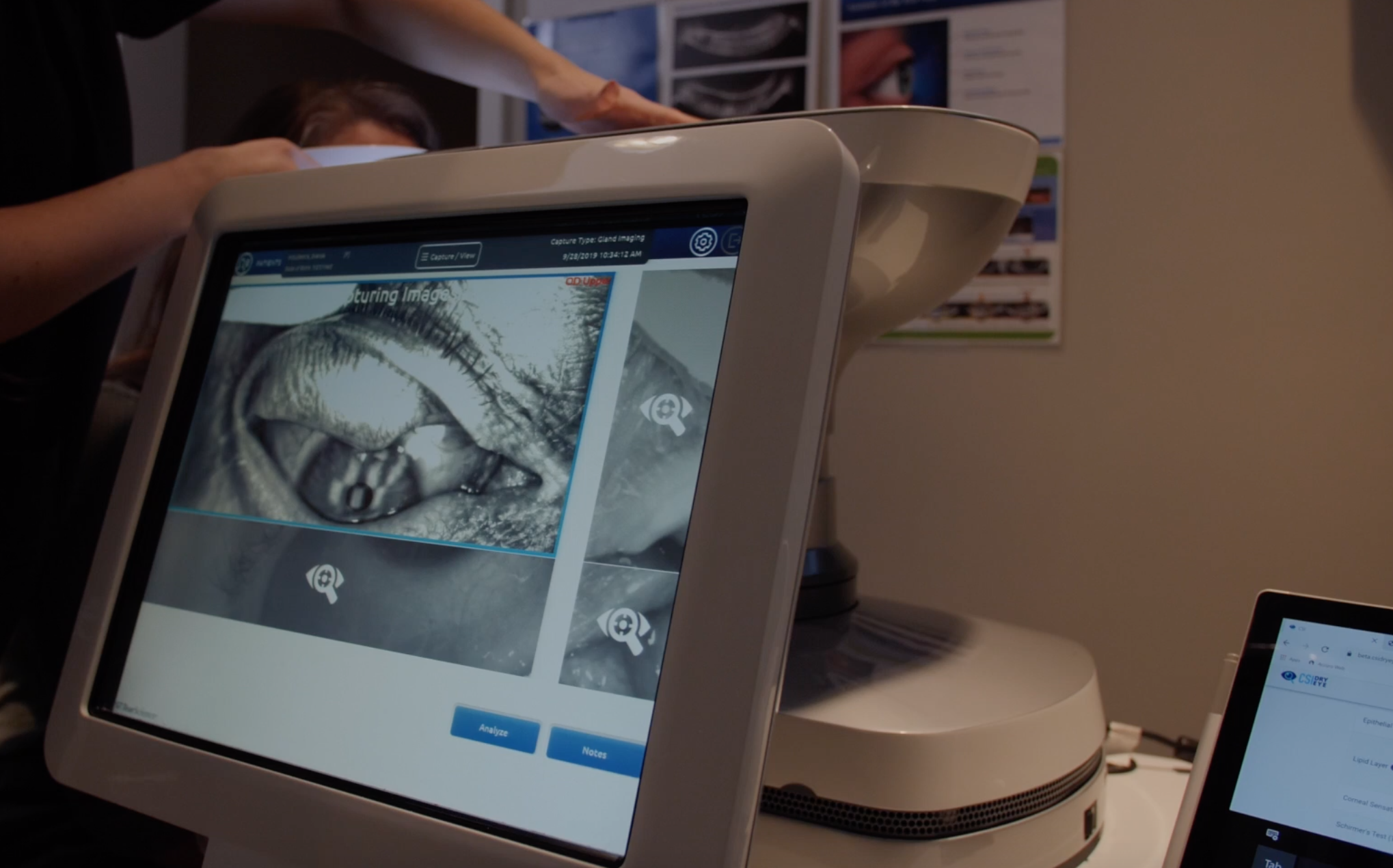
With the introduction of CSI Dry Eye technology in our practice, we have been able to help many patients have a much more objective approach to their dry eye diagnosis and management. For example, we have been able to detect countless cases where the co-conspirators were in fact shown to be quantitatively more serious than we would assess clinically. By addressing those co-conspirators, the patient symptoms dissipated which suggested that these were in fact the primary issues the patient was suffering from. We also had countless patients that we would start on therapy and despite their symptoms not improving, the objective data was suggesting an improvement. Without the data, we would have traditionally switched them to another therapy. But because the objective data suggested an improvement, we convinced the patient to continue the course and for the majority of the cases, the symptoms eventually improved as well. The Artificial Intelligence software component of CSI Dry Eye is also truly exciting. It allows us to methodically look at all these variables associated with dry eye disease in an efficient way to help us in diagnosis and understand the impact of the treatments we introduce to our patients.
We, as doctors, are excited by the fact that we have great options now and in the future for treating dry eye disease. Because of this disease’s multifactorial nature, however, there has never been a more important time than now to ensure that we develop a consistent data-driven approach to diagnosing and managing dry eye disease. Such an approach however, needs to be practical, efficient, and reproducible. CSI Dry Eye achieves that for our patients, doctors, and overall centre.